How Antimicrobial Resistance (AMR) Became a National Development Priority in India
Antimicrobial Resistance (AMR) is no longer just a medical issue—it has evolved into a national development priority for India, influencing public health, economic productivity, agriculture, environment, and governance structures.
Introduction
• Antimicrobial Resistance (AMR) refers to the ability of microbes such as bacteria, fungi, viruses and parasites to resist the effects of medicines that once successfully treated them. It is increasingly recognised as a major global health and development challenge, with estimates projecting over 10 million deaths annually by 2050 if not controlled.
• In India, AMR contributes substantially to the burden of infectious disease, compounded by high antibiotic consumption in humans, livestock, aquaculture and agriculture. Recent assessments highlight that over 60 percent of common pathogens in tertiary hospitals show resistance to first-line antibiotics, while antibiotic residues and resistant organisms circulate widely through water systems, soil, livestock and food chains.
• As these pressures intersect with economic productivity, healthcare costs, global trade, agricultural output and environmental sustainability, AMR has clearly moved beyond a technical medical concern to a national development priority requiring a comprehensive One Health approach.
1. AMR as a Public Health and Human Capital Challenge
Rising clinical treatment failures and health system burden
• Increasing resistance among pathogens such as Klebsiella pneumoniae, E. coli, Acinetobacter and Staphylococcus aureus has led to higher mortality in ICUs and a shift toward expensive last-resort drugs.
• For example, the spread of carbapenem-resistant organisms in major hospitals has resulted in prolonged hospital stays and higher treatment costs, reducing the quality of health outcomes and straining public hospitals.
• Initiatives such as the Indian Council of Medical Research’s surveillance network and national infection prevention protocols reflect efforts to reduce clinical AMR burden.
Impact on India’s human capital and economic productivity
• Frequent treatment failures in infectious diseases impact labour productivity, particularly in informal sectors where daily wage workers lose income due to prolonged illness.
• A study on AMR’s economic impact highlights that drug-resistant infections could push millions into poverty due to high out-of-pocket health expenditure.
• Programmes like Ayushman Bharat Health and Wellness Centres emphasise standard treatment guidelines and surveillance to strengthen primary care resilience.
Threat to maternal and child health outcomes
• Antibiotic-resistant neonatal sepsis remains a major cause of mortality in India, with studies showing high resistance to commonly used empirical regimens.
• Resistance in diarrhoeal pathogens complicates treatment in children, impacting nutrition and long-term cognitive development.
• Obstetric and neonatal care strengthening under the LaQshya initiative demonstrates the need for AMR integration into quality of care frameworks.
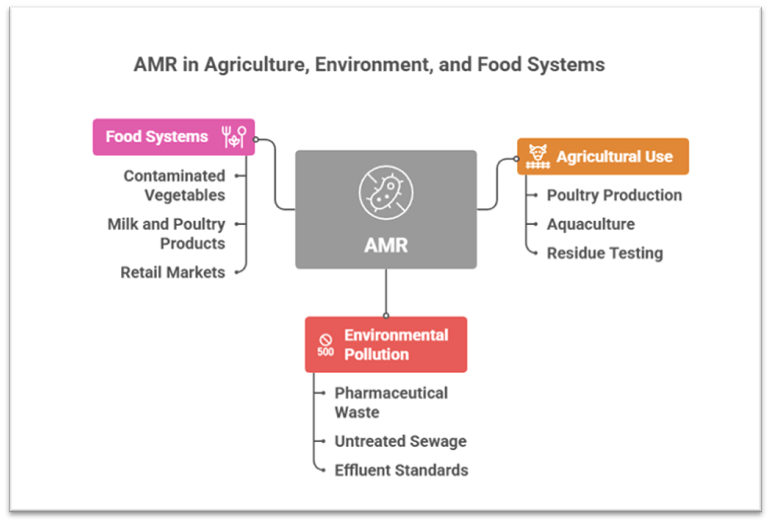
2. AMR as an Agricultural, Environmental and Food-System Challenge
Extensive antibiotic use in livestock, poultry and aquaculture impacting food safety
• India is one of the largest producers of poultry and aquaculture, where antibiotics are frequently used for growth promotion and disease prevention.
• Residues enter the food chain, raising public health risks and threatening export quality, as seen when shrimp consignments faced international rejections due to antibiotic contamination.
• Schemes such as the National Livestock Mission and fisheries monitoring programmes increasingly integrate responsible antibiotic use and residue testing.
Environmental pollution driving the spread of resistant organisms
• Wastewater from pharmaceutical manufacturing clusters, untreated sewage and hospital effluents often contain high antibiotic residues, facilitating resistant gene proliferation.
• Case study: The Patancheru–Bollaram industrial cluster showed extreme antibiotic concentrations in effluent channels, demonstrating environmental dissemination risks.
• The National Green Tribunal’s directives on effluent standards and municipal wastewater guidelines show emerging governance attempts to control environmental AMR.
Food systems as a key pathway for AMR transmission
• Contaminated vegetables irrigated with untreated wastewater, antibiotic residues in milk and poultry products and resistant bacteria in retail markets demonstrate widespread transmission routes.
• Integrated surveillance pilots across states have shown multi-sectoral linkages between human, livestock and environmental resistance patterns.
• Recent food safety regulations under the national food authority now mandate monitoring of antibiotic residues in key commodities.
3. AMR as a Governance, Development and Economic Priority
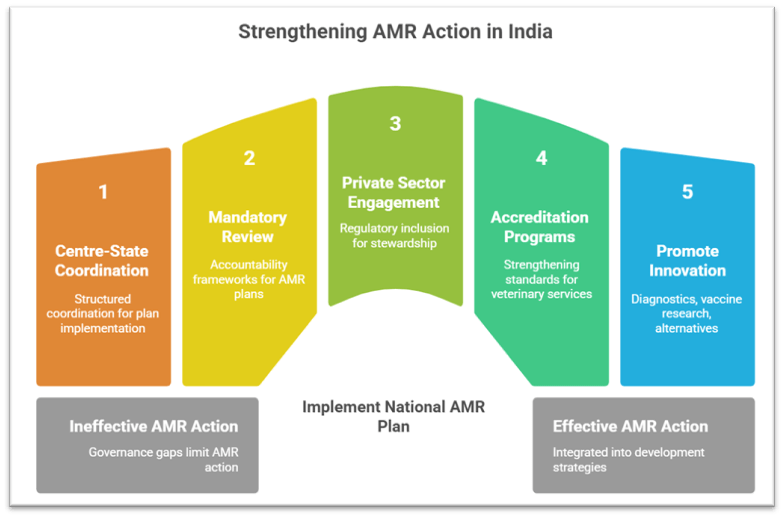
Federal governance gaps limiting effective AMR action
• Health, veterinary regulation, agriculture and waste management largely fall under State jurisdiction. Without structured Centre–State coordination, AMR plans remain uneven in implementation.
• Only a limited number of States have functional AMR Action Plans, reflecting the absence of mandatory review and accountability frameworks.
• The new National Action Plan on AMR (2025–29), which introduces national oversight and emphasises State AMR Cells, attempts to address these governance gaps.
Need for private-sector engagement across healthcare and veterinary services
• India’s private health sector provides the majority of outpatient care, making stewardship and surveillance challenging without regulatory inclusion.
• Private veterinary pharmacies and unregulated antibiotic sales contribute significantly to misuse.
• National accreditation programmes for hospitals, veterinary services strengthening under the National Animal Disease Control Programme and market-based standards represent emerging attempts to bridge this gap.
AMR as a development issue intersecting with trade, industry and innovation
• Resistance threatens export competitiveness in pharmaceuticals, marine products and food commodities due to international residue norms.
• Innovation in diagnostics, vaccine research and antibiotic alternatives is crucial for India’s bioeconomy.
• Recent initiatives promoting point-of-care diagnostics, biotechnology start-up grants and research platforms indicate AMR’s integration into broader development strategies.
Conclusion:
• Antimicrobial Resistance today represents a systemic national challenge with implications for public health, agricultural productivity, environmental sustainability, trade competitiveness and economic growth. The recognition of AMR as a national development priority is reflected in India’s intensified surveillance networks, the shift towards One Health governance and the framing of the National Action Plan (2025–29) as an implementation-oriented framework.
• However, the success of these efforts depends on robust Centre–State coordination, sustained financial incentives and effective engagement with private and informal sectors. With national estimates already indicating rising resistance in key pathogens and increasing treatment failures, India must embed AMR within its larger health and development agenda.
• If integrated governance structures, strong political commitment and multi-sectoral participation are ensured, India can achieve measurable reductions in AMR burden and position itself as a global leader in One Health-oriented development.
Recap: