Contaminated Municipal Water Supply and Its Socio-Economic Impact on the Urban Poor in India
The issue of contaminated municipal water supply in India highlights how deeply the urban poor are affected by unsafe drinking water, making their well-being the truest indicator of the nation’s public health system and governance quality.
Introduction
- Public health is not merely a measure of hospitals, doctors, or medical technology; it is fundamentally reflected in the everyday living conditions of the poorest and most vulnerable sections of society. Access to safe drinking water, alongside nutrition, sanitation, housing, and education, forms the bedrock of population health. In urban India, municipal water supply is officially classified as an “improved source,” and national household surveys indicate near-universal access to such sources across rural and urban areas.
- Yet, repeated outbreaks of water-borne diseases, episodes of mass illness, and occasional fatalities in cities reveal a deeper truth: access without quality assurance does not translate into public health security. Contaminated municipal water disproportionately affects the urban poor, who lack alternatives, thereby making their well-being a true indicator of the nation’s public health capacity and governance effectiveness.
1. Health and Human Development Implications
Disproportionate disease burden on the urban poor
- Contaminated municipal water exposes low-income urban households to water-borne diseases such as diarrhoea, jaundice, typhoid, and hepatitis, which thrive in densely populated settlements with aging pipelines and poor sewage separation.
- EXAMPLE: Recurrent outbreaks in informal settlements during monsoon seasons show how leakage between sewage and drinking water lines leads to mass infections, overwhelming public hospitals and primary health centres.
Intergenerational and nutritional consequences
- Children, pregnant women, and the elderly in poor households face higher risks of dehydration, stunting, and weakened immunity due to repeated infections caused by unsafe water. Illness during early childhood has long-term impacts on cognitive development and educational outcomes.
- CASE STUDY: Urban slum clusters reporting repeated jaundice outbreaks often also show higher school absenteeism and child malnutrition, reinforcing cycles of poverty and poor health.
Strain on public health systems and governance credibility
- Sudden spikes in water-borne illness place enormous pressure on already stretched urban public health infrastructure, diverting resources from preventive and promotive care. This erodes trust in municipal authorities and public utilities.
- Government initiative: While missions focusing on sanitation and tap connections aim to improve outcomes, gaps in monitoring and quality control undermine their public health objectives.
2. Socio-Economic and Livelihood Impacts
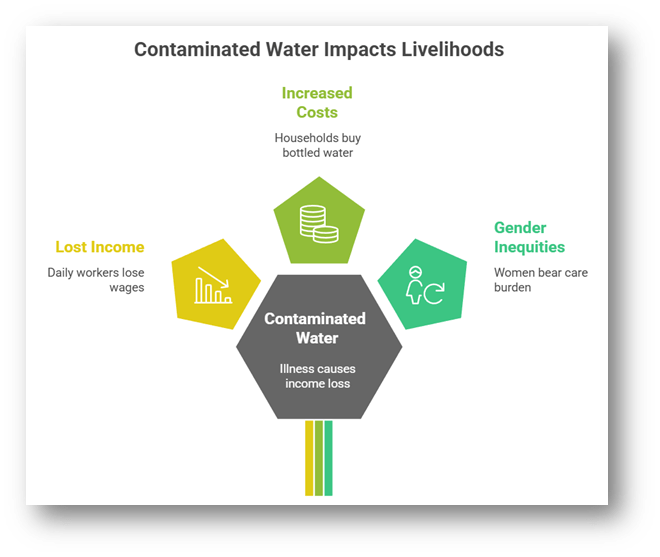
Economic vulnerability and loss of livelihoods
- For daily-wage workers, street vendors, domestic workers, and informal sector employees, illness caused by contaminated water translates directly into lost income, medical expenses, and debt. The urban poor lack health insurance buffers or paid sick leave.
- EXAMPLE: Following municipal water contamination incidents, entire neighbourhoods dependent on informal labour report income losses due to days or weeks of illness.
Increased household expenditure and coping costs
- In response to unsafe water, poor households are forced to purchase bottled water, rely on private tankers, or spend time boiling water, increasing both monetary and opportunity costs. These expenses consume a disproportionate share of household income.
- Government initiative: Despite piped water coverage under national missions, quality lapses force households to seek private substitutes, negating affordability goals.
Gendered and social inequities
- Women and girls bear the burden of caring for sick family members and managing alternative water arrangements, often at the cost of education or employment. Socially marginalized groups living in informal settlements are more exposed due to weak political voice.
- CASE STUDY: In low-income urban colonies, women often queue for tanker water after contamination alerts, increasing unpaid care work and social stress.
3. Urban Governance, Infrastructure, and Environmental Dimensions
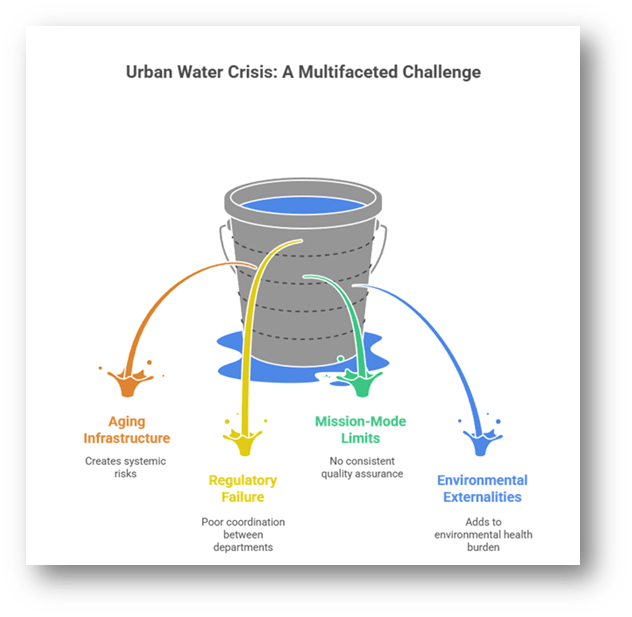
Aging infrastructure and regulatory failure
- Leaking pipelines, outdated water treatment facilities, and poor coordination between water supply and sewerage departments create systemic risks. Contamination often results from neglect rather than scarcity.
- EXAMPLE: Cities celebrated for surface cleanliness have still faced drinking water crises, highlighting the disconnect between visible sanitation and invisible water quality management.
Limits of mission-mode approaches without quality assurance
- Large-scale programmes aimed at expanding water access and sanitation have improved coverage but have not always ensured consistent water quality testing, real-time monitoring, or transparency in urban local bodies.
- Government initiative: Urban water missions emphasize infrastructure creation, but weaker enforcement of water safety standards dilutes their public health impact.
Environmental and public health externalities
- Contaminated water adds to the cumulative environmental health burden faced by the urban poor, alongside air pollution, heat stress, and inadequate housing. This compounds vulnerability and reduces urban resilience.
- CASE STUDY: Cities with high air pollution levels experiencing water contamination episodes witness compounded health impacts, particularly among slum populations living near drains and industrial zones.
Conclusion:
- The well-being of the urban poor offers the clearest lens through which a nation’s public health performance can be judged. Episodes of contaminated municipal water supply demonstrate that infrastructure expansion without quality control, monitoring, and accountability leaves the most vulnerable exposed. As India urbanizes rapidly and its population approaches the mid-century peak, reducing the burden of water-borne diseases is both a public health necessity and an economic imperative.
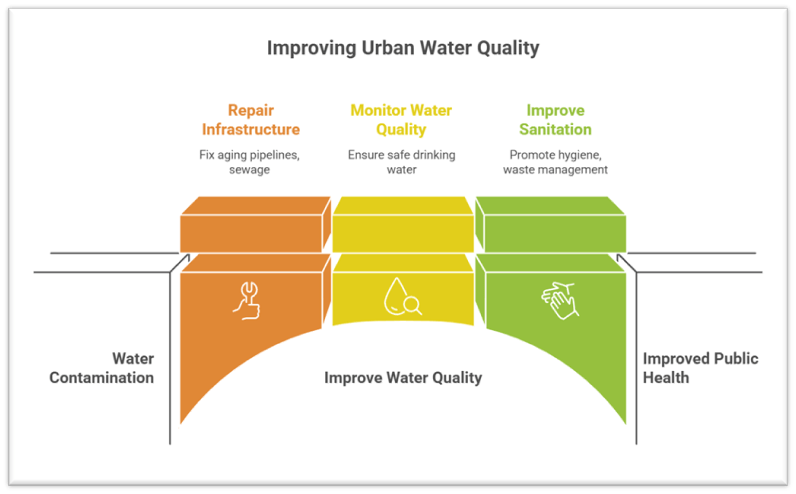
- The way forward lies in strengthening water quality surveillance, modernizing urban infrastructure, enforcing environmental and public health regulations, and empowering local governments with technical and financial capacity.
- Integrating health outcomes into urban planning, alongside sustained awareness campaigns, can ensure that access to water also guarantees safety. Protecting the urban poor from unsafe drinking water is not welfare—it is an investment in human capital, social stability, and the credibility of India’s development trajectory.
- The well-being of the urban poor offers the clearest lens through which a nation’s public health performance can be judged. Episodes of contaminated municipal water supply demonstrate that infrastructure expansion without quality control, monitoring, and accountability leaves the most vulnerable exposed. As India urbanizes rapidly and its population approaches the mid-century peak, reducing the burden of water-borne diseases is both a public health necessity and an economic imperative.
- The way forward lies in strengthening water quality surveillance, modernizing urban infrastructure, enforcing environmental and public health regulations, and empowering local governments with technical and financial capacity.
- Integrating health outcomes into urban planning, alongside sustained awareness campaigns, can ensure that access to water also guarantees safety. Protecting the urban poor from unsafe drinking water is not welfare—it is an investment in human capital, social stability, and the credibility of India’s development trajectory.
Recap: